Table of contents
Key Takeaways
-
Pharmaceutical manufacturers’ on time, in full (OTIF) rates have fallen off dramatically since the beginning of the COVID-19 pandemic, according to IDC.
-
About two-thirds of pharma supply chain companies have lost the ability to effectivity forecast demand.
-
Responses to supply chain disruptions should be timely, resilient, reliable, and compliant.
COVID-19 has taken a major toll on the pharma industry’s ability to get medicines to patients on time and in full—and a lack of patient-centric supply chain strategies may be to blame—according to a new survey report from IDC.
“Prior to 2020, almost three quarters of manufacturers said their on-time, in-full [rate] exceeded 98 percent,” explains IDC Program Vice President and Supply Chain Strategies Practice Leader Simon Ellis, who presents the survey results in a new TraceLink on-demand webinar. “In 2020, it's fallen to 28 percent. That is a massive degradation of performance and we've seen it be quite persistent over the course of 2020.”
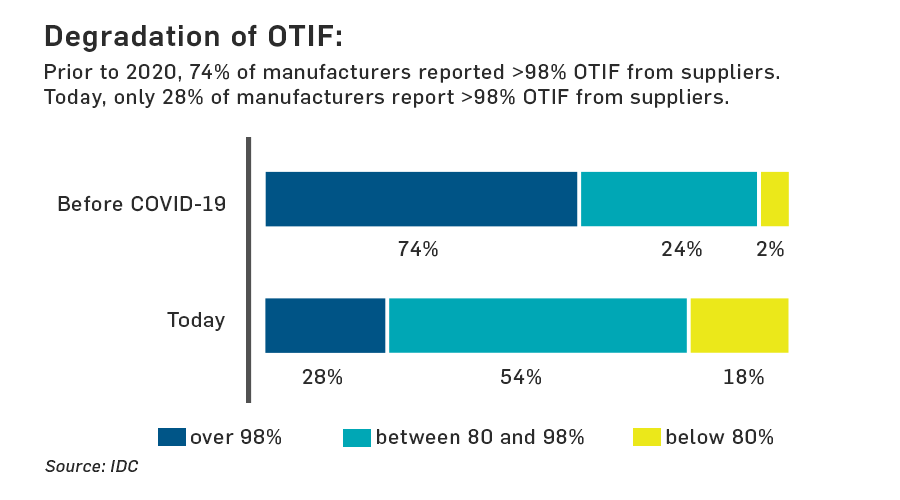
The IDC and TraceLink survey of more than 500 companies across the end-to-end pharma supply chain reveals that some additional challenges created by COVID-19 include increased production and general supply chain costs, a rise in drug shortages, and a degradation of service levels to patients. The survey also finds that:
- 81% of respondents are reactive and expediting to meet demand.
- 66% of respondents have lost the ability to forecast demand.
- 65% of respondents can no longer accurately plan supply.
Taken together, these issues indicate a clear need for companies to adopt outside-in, patient-centric supply chain management strategies and take immediate steps to boost resiliency, according to Ellis and TraceLink Digital Transformation Strategist Roddy Martin, who co-hosts the webinar. Today, only 10% of pharma companies are actively embracing patient-centric approaches.
The path to a patient-centric supply chain
How can companies get started on building a patient-centric, agile supply chain? One approach begins with an honest look at the gaps in an organization’s technology stack, says Martin.
“Start off by looking at your technology model,” he advises. “If you can't share data, if you don't have visibility of product flow, if you don't have secure distribution of your products because you don't have serialization, guess what: You've got a lot of really fundamental, basic problems to solve before you worry about patient-centricity.”
Some of Ellis and Martin’s additional recommendations for achieving patient-centricity include:
-
Deploy agile processes along with an enabling technology that supports end-to-end supply chain collaboration, actionable visibility, and data sharing between partners inside and outside the organization and across all stakeholder functions.
-
Work to ensure holistic responses to disruptions that are timely, resilient, reliable, and compliant. Additionally, do your best to ensure that the responses to disruptions minimize the impact on patient supply.
-
Begin using third-party, multi-enterprise networks to exchange information and collaborate with downstream and upstream trading partners.
-
Use “outside-in” patient dispensing and usage data on a significant scale to gain more visibility into structured segments of downstream demand and improve demand forecast accuracy.
-
Take the necessary steps to ensure that patients get the medicines they need when they need them. This must be the company-wide vision and operating model orchestrated cross-functionally across internal departments and the end-to-end demand and supply network.
“It's got to be the operating model, cross functionally, upstream to suppliers, downstream to customers, thinking about the end-to-end supply network, certainly, but the end-to-end demand network as well,” Ellis says. “Unless you do those kinds of things, you're not patient-centric. You're not patient-driven.”
Want to learn more? Watch our on-demand webinar for more IDC survey results and analysis.